How Pitt Psychiatry Meets the Complex and Evolving Behavioral Health Care Needs of Older Patients
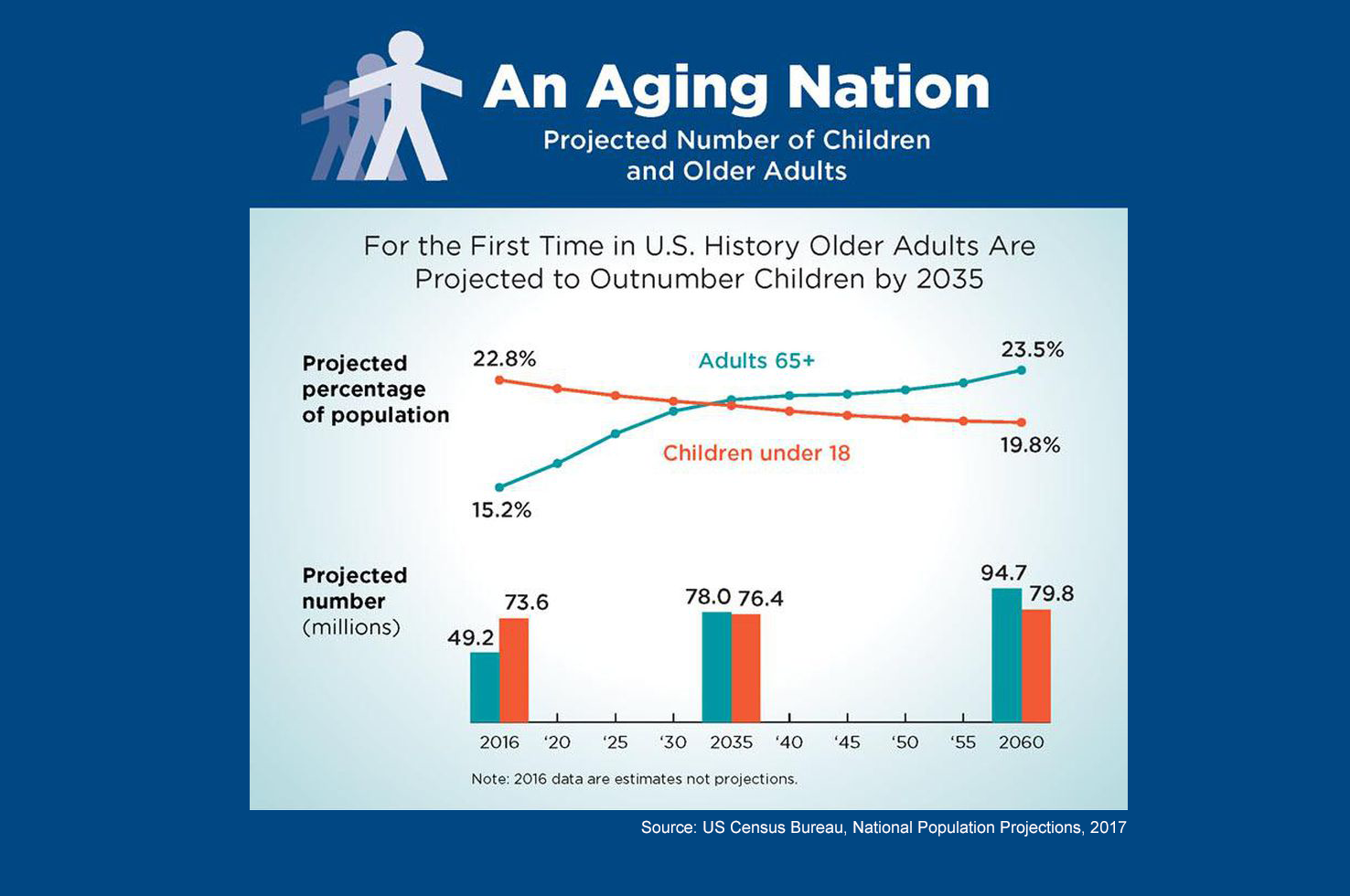
Skilled and compassionate clinicians and researchers at the Pitt Department of Psychiatry have developed innovative models of care in geriatric psychiatry, as well as training programs that prepare behavioral health care providers to deliver treatment tailored to the specific needs of older adults. Two essential components of effective geriatric psychiatry treatment—access and trust—are key concepts that guide our approach to behavioral health care for an aging population.
Below is a look at what’s happening in geriatric psychiatry at Pitt Psychiatry and UPMC Western Psychiatric Hospital (WPH).
OLDER ADULTS AT RISK FOR SUICIDE
Older people are at elevated risk for suicide, a troubling fact that is compounded for individuals over the age of 65 who also experience physical pain and/or depression. Living in a rural area further increases the risk of suicide.
Most older adults receive care for both depression and pain in the primary care setting, yet primary care physicians (PCPs) often report feeling unprepared to address the complexity of these conditions. While clinical assistance by mental health care providers can help, PCPs in rural areas usually have limited access to such collaborative opportunities.
Dr. Jordan Karp leads PREDICTOR: Pharmacy Identification and Primary Care Intervention of Older Adults at Risk for Suicide, a study funded by the American Foundation for Suicide Prevention. PREDICTOR was designed to address some of the specific needs of older patients who use both antidepressants and opioid pain relief medications, and support their PCPs, particularly in rural areas.
In the PREDICTOR study, Dr. Karp and his colleagues have identified strategies that can potentially help both patients and physicians: engaging pharmacists in focused screening of older customers flagged for receiving prescriptions for both an opioid analgesic and an antidepressant, and implementing a mental health consultation approach that blends psychiatric decision support for the PCP with care coordination. The research team targeted community pharmacists because they are accessible, even in rural areas, and are among the most trusted health care professionals. According to Dr. Karp, “Rural older adults live with both a greater medical burden and other social determinants of worse mental and physical health and suicide outcomes than older adults in urban areas. We need to identify innovative approaches to identify at-risk patients, and include other highly trusted healthcare professionals, like community pharmacists, into cutting-edge care teams.”
MEETING MEDICAL AND PSYCHIATRIC NEEDS
Historically, nursing homes were created for individuals who require skilled nursing or long-term care. Unfortunately, nursing homes are often not equipped to address the mental health needs of their patients, leaving many to languish in inpatient mental health or medical units, or simply not receive the care they require. “This population, with both medical and psychiatric needs, can be particularly challenging to place,” says Dr. Mandayam Sujata, a psychiatrist at WPH.
Responding to a lack of facilities able to provide such care, WPH collaborated with Allegheny County to establish the Kane Behavioral Unit, a nursing home unit that specializes in treatment for mental health patients whose needs require services on par with nursing home facilities. “It is a niche population, and the Kane Behavioral Unit is a safe place where they can get routine medical and psychiatric care,” said Dr. Sujata. In the last 20 months, the Kane Behavioral Unit has helped decrease the length of stay on inpatient units and successfully achieved significant stabilization of patients’ mental and medical conditions. “If they did not have this level of care, they would probably be homeless, or require round-the-clock care at home, which can be a tremendous challenge for some families” said Dr. Sujata.
THE IMPORTANCE OF TRUST
Dr. Ellen Whyte oversees WPH’s integrated geriatric behavioral health program in primary care. During the last four years, embedded LCSW therapists and geriatric psychiatrists have helped PCPs manage the complex interactions between physical and mental health care. In the integrated model, patients can receive an early assessment to determine whether they need a higher level of care or can be treated in the primary care setting—in which a therapist works with the patient in collaboration with the psychiatrist and PCP.
To improve the standard of care in the primary setting, Dr. Whyte and her team used a four-year grant through the Health Resources & Services Administration to train primary care office staff, at every level, on the basics of geriatric mental health, including how to assess for suicide risk and late-life substance abuse. This model helps older patients maintain consistent access to behavioral health care and supports PCPs who may not be prepared to provide this vital service. “We have found that our patients particularly like this model,” says Dr. Whyte. “As some research has shown, older adults prefer to be seen by primary care physicians they trust, in a setting where they are comfortable.”
The integrated behavioral health program will be enhanced by a new consultation program developed by Dr. Marie Anne Gebara. The Geriatric Research, Education, and Treatment for Mental Health (GREAT-MH) program aims to facilitate access to mental health in underserved areas. Dr. Gebara will meet with older patients in community-based settings for assessment of cognition and behavioral health symptoms, and work with PCPs to develop treatment plans and attempt to increase community knowledge about clinical and translational research programs in geriatric mental health at WPH.
THE GERIATRIC PSYCHIATRY FELLOWSHIP PROGRAM
The Department of Psychiatry also offers the UPMC Geriatric Psychiatry Clinical Fellowship, one of the most respected geriatric psychiatry training programs in the country. The one-year program is fully accredited by the Accreditation Council for Graduate Medical Education and provides a rich blend of inpatient, consultation-liaison, ambulatory, specialty setting, and VA training opportunities, along with intensive mentoring and scholarly development. In addition, the Geriatric Psychiatry Fellowship allows fellows to access an in-depth understanding of the family and environmental systems that are critical to achieving a nuanced understanding of the behavioral health needs of older patients. According to Dr. Karp, the fellowship’s director, “By 2030, there will be 8.2 million people living with Alzheimer’s and related dementias, and among all older adults, 10% to 15% have clinically significant depressive symptoms, which may present differently from younger adults and require unique medication, neuromodulation, and psychosocial interventions. Given that there are currently fewer than 2,000 board-certified geriatric psychiatrists in the United States, we must valiantly continue to both grow the field of geriatric psychiatry subspecialists and implement novel training programs for non-geriatric trained mental health clinicians and clinicians from other specialties to meet these clinical and public health needs.”
